Helping Patients With Müllerian Anomalies Navigate Care

By Lindsay Kenton, Clinical Practice Today
During pregnancy, Müllerian ducts in a developing fetus undergo changes to become the mature female reproductive tract. When they do not properly develop, conditions known as Müllerian anomalies may be present at a child’s birth, but they are often not discovered until much later in life.
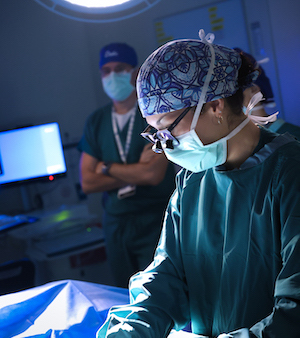
Providers with Duke Ob/Gyn’s Müllerian Anomalies Program help patients to navigate questions around their condition and determine their best options for relieving symptoms and addressing concerns, such as painful intercourse, menstrual leakage and potential pregnancy and delivery issues.
Obstetrician-gynecologists Cassandra Kisby, MD, MS; and Alison Weidner, MD, MMCi, urogynecologists and reconstructive pelvic surgeons; and Jennifer Howell, MD, a pediatric and adolescent gynecologist, comprise this comprehensive team of congenital genitourinary anomaly specialists at Duke.
By collaborating closely with urologists, colorectal surgeons and pediatric and adolescent gynecologists, the team determines how to safely and effectively offer appropriate patients innovative therapies, including vaginal dilation, vaginoplasty, vaginal septum surgery and pelvic floor physical therapy.
“Often in these cases, patients don’t expeditiously get answers for why they have pain until they come to a provider who has extensive experience with diagnosing and treating it,” Dr. Kisby said. “It’s important for providers to know to look for issues with the kidney, bladder and urethra, which can form congenitally along with the Müllerian anomaly.”
The related conditions that Duke experts treat include:
- Vaginal anomalies: Vaginal agenesis (absence), vaginal septum (longitudinal, transverse or oblique)
- Uterine abnormalities: uterus didelphys (double uterus), arcuate uterus (curved), unicornuate uterus (one-sided), bicornuate uterus (heart-shaped), septate uterus (partitioned) and absent uterus
- Mayer-Rokitansky-Küster-Hauser (MRKH) Syndrome, an undeveloped uterus and upper vagina with external genitalia that appear normal
- Obstructed hemivagina and ipsilateral renal anomaly (OHVIRA), which includes uterus didelphys, unilateral low vaginal obstruction and same-sided absence of a kidney
Q&A
How have treatment options for patients with congenital anomalies changed over the past 10 years?
Dr. Kisby: One of the greatest advances in treatment of congenital anatomic differences of the genitourinary (GU) tract is our focus on multidisciplinary care. If we focus on treatment of one condition — congenital absence of the vagina — we have seen an increasing breadth of providers who treat this condition. This is important because patients may not receive a timely diagnosis if their care provider is not familiar with Müllerian abnormalities. A handful of providers from gynecology, urogynecology, reproductive endocrinology and infertility, urology and pediatrics have increasingly focused their training on medically and surgically caring for women with these abnormalities, leading to development of magnet centers and service lines. Naturally, this has led to advances in treatment options. Going back to our example of vaginal agenesis, three types of neovagina surgeries have been around for decades. In the last 10 years, we have modified the techniques to be minimally invasive, allow for different types of grafts (split thickness, buccal, biologic), involve customized molds (described below) and open the door for innovative regenerative reconstructive options in the future.
What’s on the horizon?
When neovaginal surgeries were first described, the importance of a postoperative vaginal mold was well-established. This mold, however, was made from many different materials over the years. Initially, a hollow, cylindrical piece of glass was placed in the vagina during convalescence. As you could imagine, glass and other high-density materials could be uncomfortable, as well as put undue pressure on nearby organs. In fact, urethral and rectal fistulas were not uncommon when cylindrical hard molds were used. We have begun to design wearable vaginal molds that are more anatomic and patient friendly. One such effort is the creation of a 3D-printed vaginal mold, which continues to evolve. This mold is an alternative to the limited commercially available molds today and allows for customization to user anatomy. With 3D printers becoming more widely accessible, we believe this method could become universally accepted, with hopes of contributing to increased patient satisfaction and decreased complications.
How do you hope this will impact urogynecology and reconstructive pelvic surgery fellowship training in the future?
It is an exciting time at Duke, because we are able to holistically and comprehensively care for patients with GU abnormalities using a team-based approach, a team that actively involves our trainees. Our group has purposefully made trainee education a priority in building this service line. We regularly invite trainees outside our individual subspecialties to participate in medical decision making and surgical intervention. For these fellows, congenital abnormalities is an education milestone — what better way to learn than from a growing multidisciplinary team?
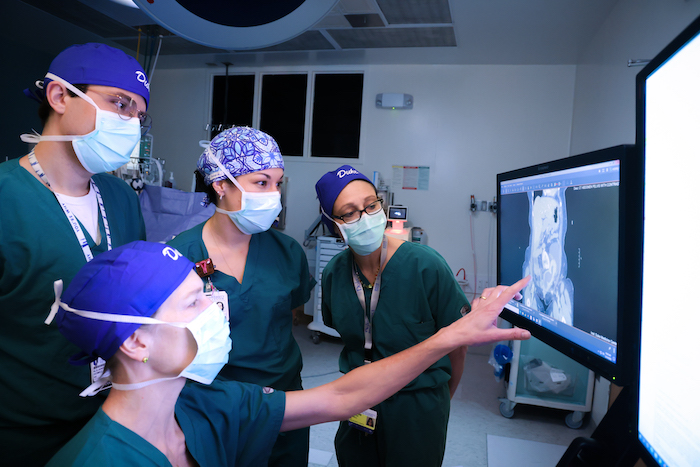
What are the unique aspects of being part of this comprehensive team?
Dr. Weidner: Müllerian anomalies are but one example of a wide range of congenital pelvic conditions that can have complex ramifications for patients across multiple organ systems. Often our patients have had reconstructive surgery early in life and, while lifesaving, these procedures sometimes need revision or can lead to other challenges as patients grow into adulthood. Many congenital pelvic and urogynecologic conditions are fairly rare, and some patients have had surgeries that are no longer common, making each situation a unique challenge — and one that benefits from broad experience and case volume. A multidisciplinary team of experienced and creative surgeons like what we offer at Duke brings the necessary skillset to offer each patient the best possible solution. We work as a team to coordinate surgical care, recovery and long-term follow-up — that’s a level of quality of care that is just not possible at most hospital centers across the country.
How does this program bridge the gap between generalists and specialists, and how does it benefit patients?
Dr. Howell: With the establishment of Pediatric and Adolescent Gynecology, patients now have a specialist care “home” where they can receive evidence-based, age-appropriate care by a knowledgeable specialist. For example, diagnoses such as imperforate hymen, transverse vaginal septum and congenital absence of a vagina can present in similar ways but are treated very differently. Patients with these differences are relatively rare (less than 1 out of 1,000). Patients who are referred to us when these conditions are suspected can receive the necessary evaluation to have the right intervention at the right time in their lives. Community obstetrician-gynecologists may not have enough familiarity to know exactly what needs to be done, given how rarely they encounter these patients, and we are able to provide our expertise.