Cervical cancer is the fourth most common cancer in women worldwide, according to the National Cancer Institute. Researchers and faculty at the Duke Center for Global Women’s Health Technologies (GWHT) have committed to addressing barriers to early detection of the disease, and mechanisms for cervical cancer screening through education, technology and cultural awareness.
In 2020, The John D. and Catherine T. MacArthur Foundation selected a proposal titled “Women-Inspired Strategies for Healthcare: A Revolution Against Cervical Cancer” as among the Top 100 out of 755 submitted in the 100&Change competition. The competition solicited proposals that promise measurable progress in solving a critical problem. The momentum of the initiative continues, with the goal being empowerment of marginalized women with knowledge, innovative clinical tools and confidence to take control of health and kickstart a worldwide movement against cervical cancer, according to leverforchange.org, a nonprofit affiliate of the MacArthur Foundation.
A Duke team behind the ongoing work outlined in the WISH initiative is comprised of Megan Huchko, MD, MPH, clinical lead; and Nimmi Ramanujam, PhD, technology lead. Drs. Huchko and Ramanujam have experience in cervical cancer prevention, technology innovation and entrepreneurship. Collectively, they have global partnerships in more than 10 countries across four continents. Dr. Huchko has a dual appointment in Ob/Gyn and the Duke Global Health Institute.
At Duke, Dr. Huchko started the Center for Global Reproductive Health to increase research collaborations and educational opportunities. The goal is to reach 5 million women in two epicenters, Peru and Kenya, and reduce deaths by 50% in five years.
Addressing barriers, impacting lives
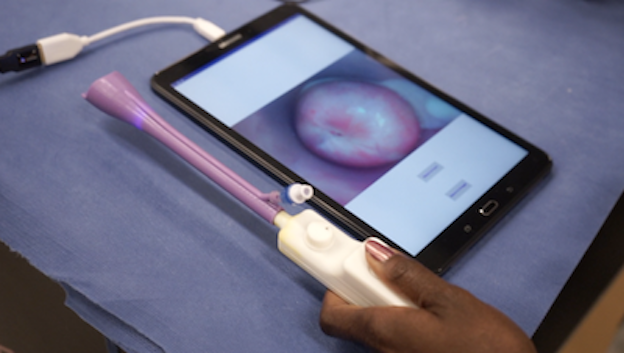
Two common key barriers to global cervical health screening are fear of the speculum and feelings of vulnerability during gynecologic exams, according to GWHT researchers. Through ongoing work at the GWHT, gynecological exams across the globe have been reimagined. Duke experts in biomedical engineering have worked collaboratively over the past decade to develop and improve novel, low-cost screening tools. The original device, the Pocket Colposcope, offered a portable, readily available and cost-efficient screening tool that could be used in primary care settings. The Pocket Colposcope is a magnified telescopic device and camera designed to allow medical professionals to look through a speculum to see the cervix. That version has undergone design modifications since first being developed a decade ago, and in 2018, the Pocket Colposcope received FDA clearance. Continual innovation led to the development of a new iteration, called the Callascope, which enables speculum-free provider insertion or self-insertion, and image capture of the cervix, according to the Calla Health Foundation.
The Callascope – human-centered design
Developed by Mercy Asiedu, PhD, when she was a graduate student at the GWHT working in Dr. Ramanujam’s lab, the Callascope has recently been updated with human-centered design in mind.
• The new version utilizes a 5 megapixel rather than a 2 megapixel camera.
• An integrated camera and shell is now utilized. The whole stem is the camera, and a removable tip functions as the introducer. The Callascope can easily go from being a speculum-free device that can be used for self-imaging (with the use of the inserter tip), to an imaging device that can be used with a speculum (without the use of the tip).
• Silicone was added to the tip to make it softer; brighter custom LEDs allow for a clearer picture of the cervix.
• The Callascope can be used in conjunction with HPV self-sampling for cervical cancer screening by the patient at home. Especially in cases where privacy is key, such as in culturally conservative regions, the Callascope allows users to take initiative and improves access to screening services. This, according to the GWHT, is life changing.
— Duke Center for Global Women’s Health Technologies
Learn more: Making Change by Changing the Callascope