In This Section
Global Health Elective Program at KCMC
Building Technology and Trust: AI Algorithms and Cervical Cancer
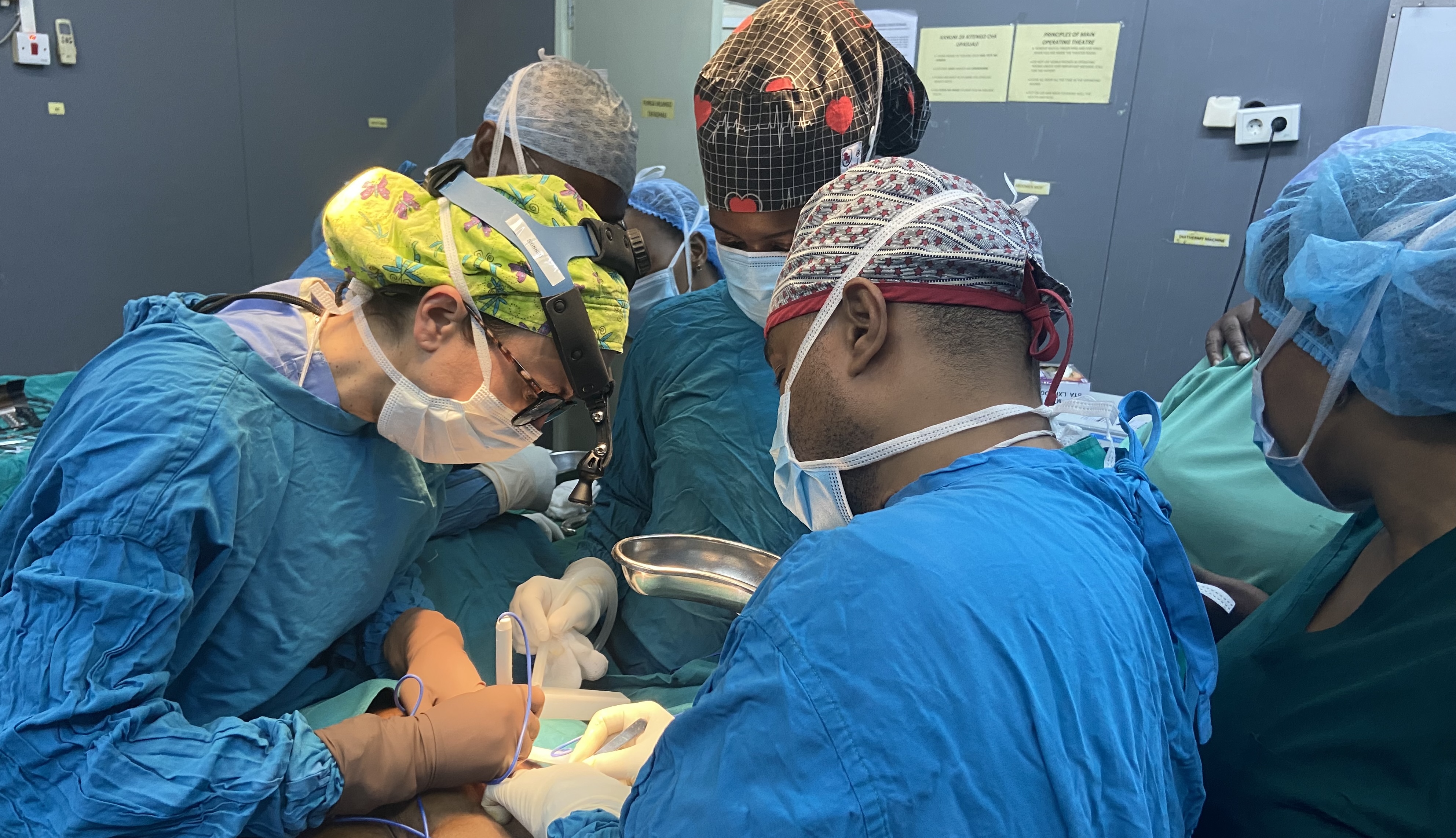
Third- and fourth-year Duke Ob/Gyn residents interested in global health careers or augmenting their training experience have the option to participate in a unique global health elective program in Moshi, Tanzania. The program comprises a comprehensive clinical and surgical experience ranging from five to six weeks in duration at Kilimanjaro Christian Medical Centre (KCMC).
For more than a decade, residents have participated in the program and grown as physicians through their immersive time in Tanzania. The curriculum includes both learning and teaching in academic, clinical and hospital settings at KCMC. The program’s full schedule of inpatient and outpatient clinical care and high surgical case volume offers a comprehensive experience throughout the elective. From generalist care in the labor and delivery setting to high-acuity gynecologic surgery cases, participants gain knowledge and experience that complements their learning at Duke University Health System (DUHS).
Residents engage and collaborate with their colleagues and co-residents at KCMC, and they have opportunities to share their scholarly work as presenters and hands-on teachers. Tumor board discussions, grand rounds, research and the opportunity to experience new and different perspectives augment the breadth of the traditional residency experience. Preparation for the global health elective includes participating in a curriculum with discussions including ethics, history of global health and site-specific cultural expectations. The program is supported by both Duke Health and KCMC faculty, with Duke Health faculty traveling with the residents. The program creates pathways and mentorship for continued work in global health after graduation from residency.
“Duke and KCMC have a special collaborative relationship that spans almost two decades, and I am honored to be part of the team,” said Duke Ob/Gyn faculty member Emily Herfel, DO, MSc- GH, who serves as the program’s director. “Together we have created projects aimed at improving women’s health outcomes. Projects include updated topics for didactic learning, and a newly added laparoscopic training curriculum that offers consistency as participants progress in their learning and skill sets. We now are building an ultrasound curriculum as the program continues to grow. Bedside and operating room hands-on teaching is my favorite part, as well as learning about cultural norms and creative patient care.” Learn more about the program at duke.is/GHE.
"My time in Moshi brought clarity to years of training, sacrifice and perseverance, grounding my education in purpose and perspective in ways no classroom ever could. I learned not only how to practice medicine with limited resources, but how to listen more closely, collaborate more intentionally and remain a student in every clinical space I entered. The generosity of the patients and clinicians who welcomed me as one of their own reshaped how I understand service, equity and responsibility. This experience has permanently influenced how I approach medicine, reminding me that global health electives are not simply enriching experiences, but formative ones.”
— Resident LaMani Adkins, MD, who spent September and October of 2025 at KCMC
"Having the opportunity to learn in a differently resourced setting while at this formative stage of training is truly invaluable and will inform how I seek to engage with international health work — and health access domestically — beyond residency. Spending my elective block at KCMC was such a privilege. Learning from and alongside ob/gyn residents there — most of whom were training far from home and many in a foreign country — was humbling, and their dedication was inspiring. I learned an incredible amount by having the opportunity to discuss management of complex gynecologic patients, scan and monitor antenatal patients and operate alongside ob/gyns who are practicing with fundamentally different constraints than exist at Duke. With enormous shifts in the global health landscape over the last year, seeing firsthand the repercussions of these changes was galvanizing for my involvement in future related work."
— Resident Alexandra Norton, MD, MPH, who spent April of 2025 at KCMC

Duke Ob/Gyn faculty Megan Huchko, MD, MPH, Hollier Family associate professor of global health, has devoted much of her career both in the U.S. and globally to conquering cervical cancer. The disease is now one of the most preventable types of gynecologic cancers, attributed to HPV vaccination and screening. Further progress continues as self-collection home testing options become available. This option enables patients who otherwise may have not been tested or diagnosed to check for the disease, then seek care before progression occurs. Access to screening, with follow-up care if precancerous or cancerous cells are detected, is imperative for progress to continue, according to Dr. Huchko. Her work in partnership with Duke’s Center for Global Reproductive Health and the Kenya Medical Research Institute (KEMRI) is creating sustainable and affordable models for early detection of this highly preventable disease.
Bringing Care Closer to Women
In Kisumu, a city in western Kenya, a team of researchers and clinicians is working to make cervical cancer screening more accessible and more human. For many women in western Kenya, health care can feel out of reach. Clinics are far apart, specialists are scarce and basic equipment is limited. These barriers mean that conditions like cervical cancer are often caught too late.
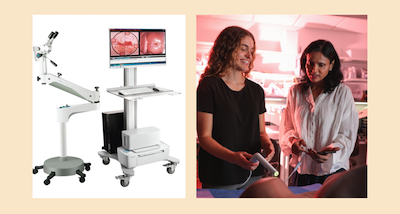
This collaboration aims to change that by introducing self-collection swabs that women can use to obtain cells that can be tested in a lab for Human Papillomavirus (HPV), the virus that causes cervical cancer — allowing women to take the first step themselves. By equipping local clinics with mobile tools that make patient and health care worker communication and scheduling of follow up care reliable.
At the clinic, providers use a handheld imaging device called the Pocket Colposcope to take detailed photos of the cervix. The images are uploaded through a mobile app, the Calla Health App (CHA), which also helps train an Artificial Intelligence (AI) algorithm to assist with diagnosis and follow-up. The Pocket Colposcope closes an important clinical gap, triaging patients who test positive for HPV.
Smarter Tools, Not Replacements
AI has the potential to level the playing field in global health. In places where trained specialists are few, AI can help ensure more consistent and accurate results.
But, as the team quickly learned, building good AI isn’t just a technical challenge: it’s a human one. Image quality varies, internet connections drop and every provider has a slightly different way of working. One common issue is blur in handheld images, which can reduce accuracy. To fix this, the team built an AI software tool that detects when an image is too blurry and alerts the provider to retake it. It also helps developers to evaluate and take into account image quality when they create and test algorithms.
The idea worked in theory, but in practice, it sometimes slowed down clinic workflow. For the researchers, that was an important reminder: real-world solutions need real-world input. Read the full article at duke.is/CC3.