
1972

Division of Gynecologic Oncology Founded
The National Cancer Institute was established in its current form by the National Cancer Act of 1971, signed into law by President Richard Nixon (above). In 1972, the Division of Gynecologic Oncology in the Department of Ob/Gyn was founded under William T. Creasman, MD (now at MUSC Women's Care in South Carolina), the division’s first chief, pictured below. This coincided with Duke becoming an officially designated Comprehensive Cancer Center by the National Cancer Institute, then under the leadership of oncologist William Shingleton, MD.

1984
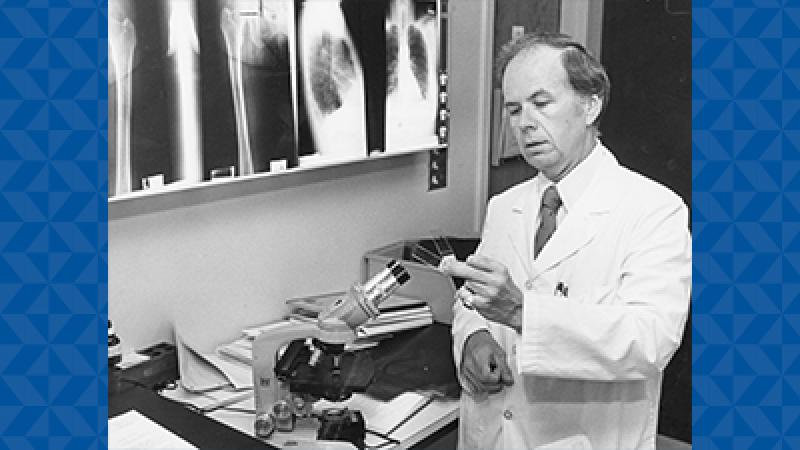
Pioneering research: prevention of post-operative venous thrombosis in gynecologic oncology
Daniel Clarke-Pearson, MD was a pioneer, along with William Creasman, MD, pictured, in the prevention of post-operative venous thrombosis in gynecologic oncology. Their key findings, with Duke co-authors Ingrid D. Synan, RN; Wanda Hinshaw, MS; and R. Edward Coleman, MD; were published in Obstetrics & Gynecology in 1984.
1986
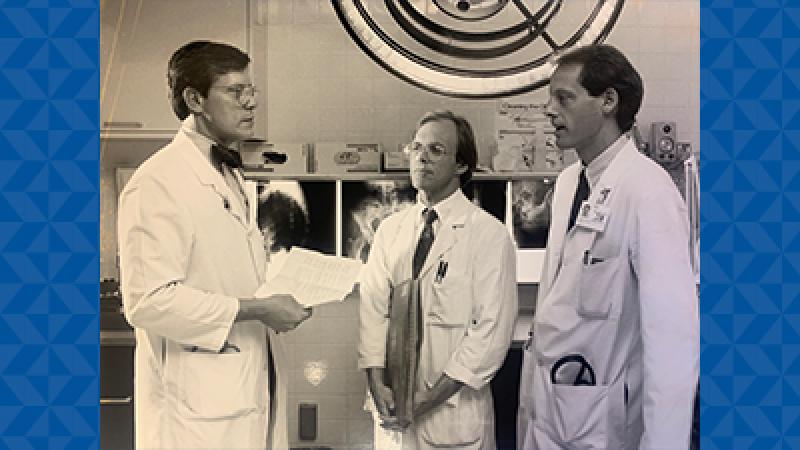
Daniel Clarke-Pearson, MD, named the next chief of the Division of Gynecologic Oncology.
1987
Development of surgical staging for uterine cancer pioneered
William Creasman, MD, who’d directed the division until 1986, led a Gynecologic Oncology Group (a national consortium of institutions and investigators) study that pioneered the development of surgical staging for uterine cancer, which included pelvic and aortic lymph node sampling. The results were published in Cancer in 1987. (Duke co-authors included C. Paul Morrow, MD; Brian Bundy, PhD; Howard Homesely, MD; James E. Graham, MD; and Paul Heller, MD.
1991
Role of over expression and mutation of the TP53 gene in epithelial ovarian cancer reported
Jeffrey Marks, PhD, and Andrew Berchuck, MD, with Duke co-authors Andrew M Davidoff; Billie Joe Kerns; Peter A. Humphrey; John C. Pence; Richard K. Dodge; Daniel Clarke-Pearson, MD; James Iglehart, MD; and Robert C Bast Jr, reported for the first time on the role of overexpression and mutation of the TP53 gene in epithelial ovarian cancer. The findings were published in Cancer Research in 1991.
1994
Mutations in the BRCA1 gene is a driver of breast and ovarian cancers discovered
1995

Duke Hereditary Breast-Ovarian Cancer Clinic Established
In 1995, Andrew Berchuck, MD, with Kelly Marcom, MD, helped establish the Duke Hereditary Breast-Ovarian Cancer Clinic.
2002
Oral contraceptives (largely due to progestin) reported to reduce the risk of ovarian cancer
Joellen M Schildkraut, PhD, MPH (now at Winship Cancer Institute) and Gustavo Rodriguez, MD (adjunct associate professor and former fellow, Duke Department of OB-GYN; director of the Division of Gynecologic Oncology, NorthShore University Health System); with Duke co-authors Brian Calingaert, MS; Polly A Marchbanks, PhD; and Patricia G Moorman, PhD, MSPH; reported that oral contraceptives (largely due to progestin) reduced the risk of ovarian cancer. Their research was published in the Journal of the National Cancer Institute in 2002.
2005

Andrew Berchuck, MD, named third chief of the Division of Gynecologic Oncology,
In 2005, Andrew Berchuck, MD, co-founded the Ovarian Cancer Association Consortium (OCAC), an international group studying the molecular epidemiology of this disease.
2008
Leadership at SGO
Dr. Berchuck served as president of the Society for Gynecologic Oncology (SGO).
2009
Implications of comparative effectiveness and quality-of-life and outcomes studies explored
Laura Havrilesky, MD, MHSc, was among the first investigators to explore the implications of comparative effectiveness and quality-of-life and outcomes studies in gynecologic oncology (Gynecologic Oncology, 2009)
2011

First comprehensive genomic analysis of ovarian cancer published
Andrew Berchuck, MD, was a member of the Cancer Genome Atlas Ovarian Cancer Working group that in 2011 published, in Nature, the first comprehensive genomic analysis of ovarian cancer.
2012

Point-of-care technologies for cervical cancer screening and diagnosis developed
In 2012, a research team led by Nimmi Ramanujam, PhD, began developing point-of-care technologies for cervical cancer screening and diagnosis. A low-cost Point of Care Tampon (Pocket) Colposcope was developed that could easily be inserted through a speculum to achieve comparable magnification and contrast to that of a standard colposcope. The goal was to achieve cervical cancer screening and detection in low-resource, limited-access primary care settings. This team also included Christopher Lam, PhD; Jenna Mueller, PhD; Marlee Krieger, MS, of the Duke Center for Global Women’s Health Technologies; and John Schmitt, MD, of Duke Ob/Gyn.
2016
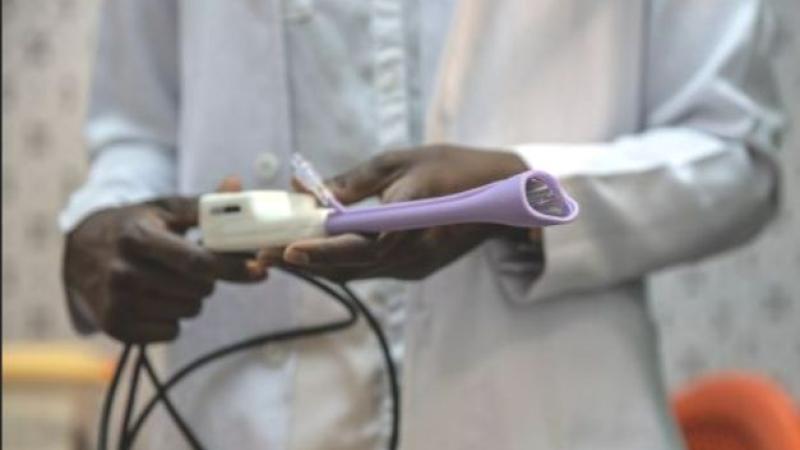
Callascope developed for the detection of cervical cancer without the need for a speculum
In 2016, to achieve the goal of self-administered screening with high-resolution images, a graduate student with the Duke Center for Global Women’s Health Technologies, Mercy Asiedu, PhD, developed the Callascope for the detection of cervical cancer without the need for a speculum. The device can be used in conjunction with HPV self-sampling for cervical cancer screening either by a clinician or by a patient in the privacy of their own home and produces high-resolution images.
2017
OAC identified 12 new genetic variants that increase the risk of developing epithelial ovarian cancer
The Ovarian Cancer Association Consortium (OCAC) (co-founded by Andrew Berchuck, MD) identified 12 new genetic variants that increase the risk of developing epithelial ovarian cancer and confirmed the association of 18 of the previously published variants. Duke authors included Andrew Berchuck, MD; and Marjorie Riggan, BS. The findings were published by Nature Genetics in 2017.
2018

Global Reproductive Health at Duke Founded
In 2018, Megan Huchko, MD, MPH, founded the Center for Global Reproductive Health at Duke to increase research collaborations and educational opportunities with the goal of reaching 5 million women in two epicenters of cervical cancer (Peru and Kenya) and reducing cervical cancer deaths by 50% in five years.
2019

Endometrial Cancer Molecularly Targeted Therapy Consortium was established
In 2019, the multi-institutional Endometrial Cancer Molecularly Targeted Therapy Consortium was established with a $1 million Kay Yow Cancer Fund/V Foundation for Cancer Research grant to Angeles Alvarez Secord, MD, MHSc, and Duke Cancer Institute. This national group is focused on research into molecular alterations and targeted biological therapies in endometrial cancer.
2020
Pocket Colposcope was optimized for commercialization
In 2020, the Pocket Colposcope was optimized for commercialization in collaboration with a product design and development company. The device is now commercially available.
2020

Angeles Alvarez Secord, MD,MHSc, was named SGO President
In 2021, Angeles Alvarez Secord, MD,MHSc, was named president of the Society for Gynecologic Oncology (SGO) for the 2023-24 term.
2021

Haley Moss, MD, MBA, named the first-ever director of the Breast and Gynecologic Oncology System of Excellence,
In 2021, Haley Moss, MD, MBA, was named the first-ever director of the Breast and Gynecologic Oncology System of Excellence, U.S. Dept. of Veterans Affairs National Oncology Program (NOP). She’s working to expand access to care for women veterans through tele-oncology and clinical trials.
2021

Novel collaboration between the Duke Cancer Institute Supportive Care & Survivorship Center and the Duke Fertility Center helps cancer patients' family-dreams come true.
In 2021, Duke Ob/Gyn opened a new, state-of-the-art fertility center. For more than 25 years, Duke Fertility Center has been a nationwide leader in fertility services. Among the therapies available are onco-fertility, bringing together oncology and reproductive endocrinology specialties to maximize the reproductive potential of cancer patients and survivors. This novel collaboration between the Duke Cancer Institute Supportive Care & Survivorship Center and the Duke Fertility Center is helping cancer patients' family-dreams come true.
2022

Gyn Onc faculty directs Quality and Safety Fellowship
In 2022, the division welcomed the first Quality and Safety in Women’s Health Fellow. The program is being directed by Laura Havrilesky, MD, MHSc.
2022

Duke Researchers Develop Prediction Model for Opioid Prescribing Following Gynecological Surgery
Brittany Davidson, MD, with Laura J. Havrilesky, MD, MHSc, and several current and former residents developed a model to predict individualized estimates of outpatient opioid use post-operatively (at hospital discharge) for a broad range of patients undergoing gynecologic surgery; published in 2022 in the Journal of the American Medical Association (JAMA) Open Network.